“Why are you so harsh on yourself?” 😳
I got a DM on Instagram recently, where the (probably) well-meaning person asked something along the lines with “why are you so harsh on yourself when it comes to diabetes?” 😳
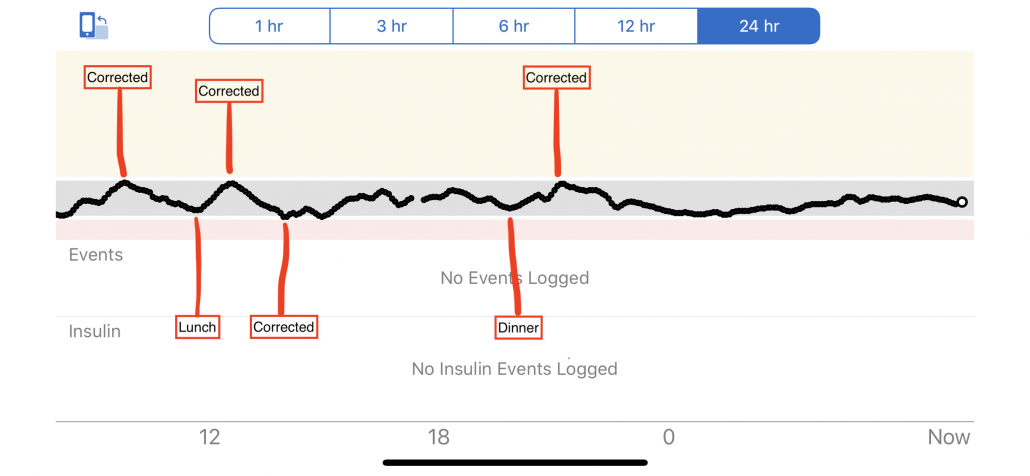
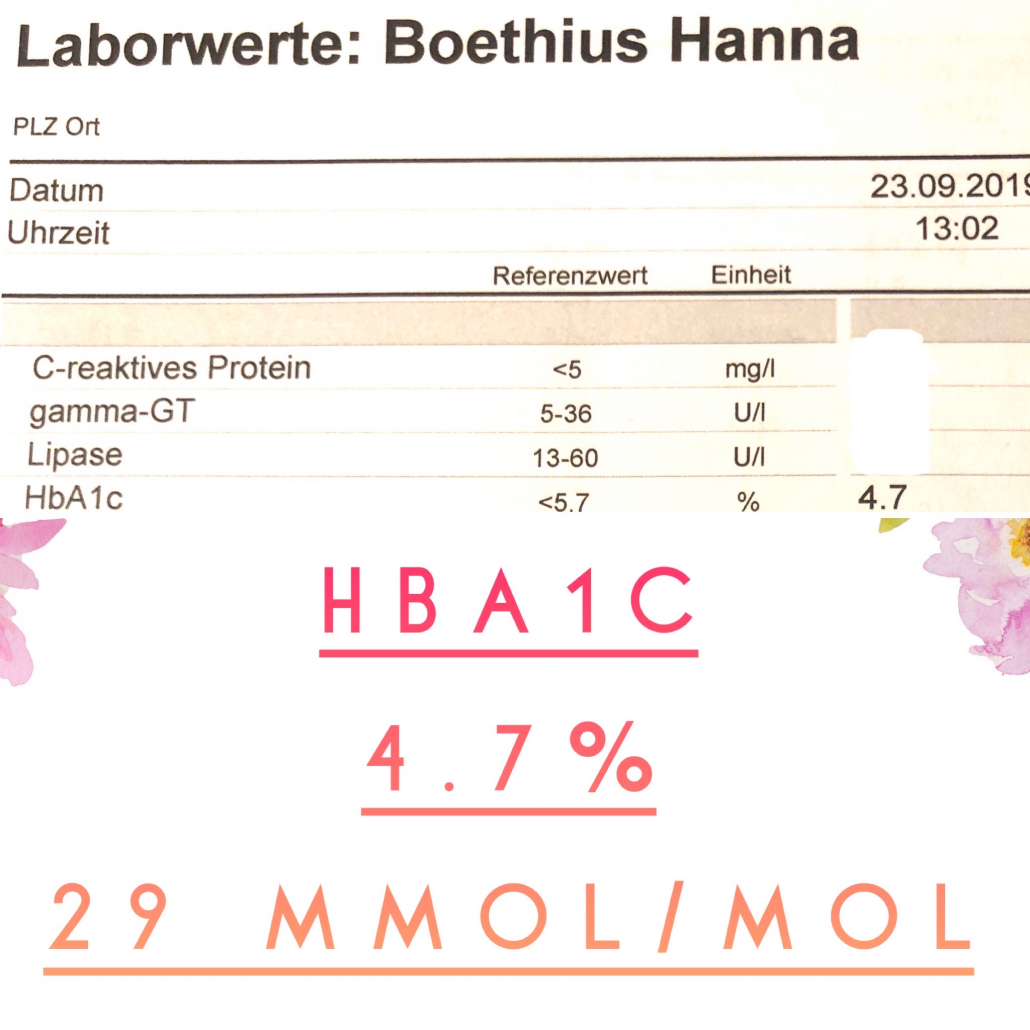
It was implied that I pay too much attention to things like blood sugars, nutrition and HbA1c, when “all you have to do is count carbs and cover for them with insulin.”
Well. I don’t agree. 🤷🏻♀️ To me, that is a way too simplistic way of looking at managing something as individual as diabetes can be. Check out the rest of my answer in this short clip:
👉🏼 What tools have you found that work the best for you in your diabetes management? 👈🏼
The only purpose of this video and website is to educate and to inform. It is no substitute for professional care by a doctor or other qualified medical professional. This video and website is provided on the understanding that it does not constitute medical or other professional advice or services. Instead, we encourage you to discuss your options with a health care provider who specializes in treating Type 1 Diabetes.